How it works
Ultrasound uses high frequency sound waves (3 to 17 megaHertz) to form images based on the reflectivity of tissue interfaces. At the interfaces between different types of tissue, some of the sound waves are reflected back to the ultrasound probe. The delay between the transmission of the sound waves and this echo reaching the probe allows the ultrasound machine to calculate the depth in the body from which this echo is coming from, and uses this information to build up an image. In practice, this process is so rapid that a real-time image is formed on the ultrasound screen.
Ultrasound waves are not transmitted through air, therefore the ultrasound probe must be ‘coupled’ to the patient’s skin using a gel.
Ultrasound is a relatively quick and inexpensive imaging tool, and has a wide range of useful applications in the assessment of hepatobiliary, renal, gynaecological, obstetric, thyroid, testicular and rheumatological pathology. Because it provides real-time needle visualization, it is ideally suited for guiding biopsies. By using the Doppler principle, ultrasound can also be used to identify the presence and velocity of blood flow, which makes it very useful in the evaluation of arteries and veins.
Ultrasound has no known adverse effects on humans, giving it a huge advantage over other imaging techniques. Its main limitation is that it cannot see through air or calcium, therefore it cannot be used to evaluate the lungs, GI tract or bones.
Ultrasound differs significantly from other imaging modalities in that the quality of the images produced is extremely operator dependent; the stored images that are sent to PACS are merely representative stills from a dynamic scan that has been interpreted in real-time by the sonographer. As a result, medical students often find it much more difficult to understand ultrasound images compared to xrays, CT and MR images. Do not despair – with a little bit of effort on your part, you will have a much better understanding by the end of your rotation.
Ultrasound at SVUH
There are 9 ultrasound scanning rooms in the department, six of which are used for diagnostic ultrasound. One room is designated the ultrasound procedure room, where ultrasound-guided biopsies (e.g. liver, prostate, renal, lymph node, and thyroid biopsies or fine needle aspirations) and drainages (e.g. pleural effusions, ascites) are performed. There are two additional rooms that are dedicated to prostate biopsy.
There are two further portable ultrasound scanners in the department, which are used for guidance for procedures in the Interventional Radiology suites and for portable diagnostic ultrasound in the ICU.
Most of our ultrasound scanning machines have a selection of ultrasound probes available for use, depending on the examination being performed. These probes differ in the frequency of sound waves they produce, and also in their shape (curved, providing a wide field of view, and linear, giving a narrower field of view). As a general principle, the lower the frequency of
sound waves used, the deeper into the body the ultrasound machine can image. However, this comes with a trade-off; lower frequency probes produce lower resolution images. Nonetheless, they are ideally suited for imaging the abdominal organs, urinary tract and female pelvis.
Higher frequency (typically linear in shape) probes are therefore used to image more superficial structures, providing very high resolution images. This makes them ideal for assessment of structures such as the carotid arteries, as well as cervical or inguinal lymph nodes, the thyroid gland, the testes, tendons and most joints.
Commonly-performed Ultrasound Examinations
Ultrasound abdomen
This is one of the most frequently requested ultrasound examinations. It is a fast and inexpensive way of assessing the liver for evidence of cirrhosis, for identifying focal liver lesions such as HCC or metastases, and for diagnosing gallstones and dilatation of the bile ducts. The portal vein can be assessed with Doppler ultrasound for thrombosis, or for reversal of flow (which may occur in chronic liver disease). Splenomegaly can be diagnosed. Pancreatic neoplasms are occasionally diagnosed at ultrasound, however they can be subtle and CT is generally performed when there is a suspicion of pancreatic cancer.
Ultrasound kidneys
We use this to assess renal size (the kidneys may be atrophic in chronic renal failure), to identify calculi, hydronephrosis and focal renal lesions; renal cysts are the most common focal lesions identified.
Ultrasound pelvis
This is an excellent first-line test when gynaecological pathology is suspected. Ultrasound can diagnose ovarian cysts and neoplasms, uterine fibroids and endometrial cancer. It is usually performed transabdominally, with a full bladder (the patient’s) which acts as a ‘window’ into the pelvis. Occasionally, we need to see the uterus or ovaries in finer detail – to do this, we can use a higher frequency probe passed into the vagina (transvaginal ultrasound) so that the probe can be positioned as close to the pelvic organs as possible.
Ultrasound aorta
This is a very quick and easy way of diagnosing abdominal aortic aneurysms.
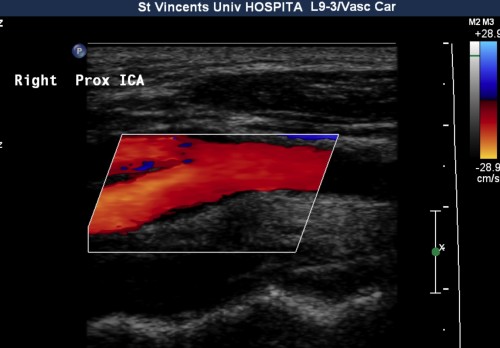
Ultrasound carotids
Using Doppler ultrasound, we can measure the velocity of blood flow through areas of atherosclerosis in the carotid arteries, and use the measurement to calculate the percentage stenosis of the artery. This is typically performed in any patient who has had a TIA or CVA.
Ultrasound Doppler Venogram
This can be used to diagnose DVT in the upper or lower limbs. While we use colour Doppler to look at blood flow in the veins, the most sensitive method for detecting a DVT is to push on the vein with the probe, and see if it compresses – if there’s thrombus there, we can’t compress it.
Ultrasound ‘Ducts and Dopplers’
This is used to assess the patency of the hepatic artery, portal vein, hepatic veins and common bile duct in patients who have had a liver transplant. It is always performed the day after transplantation, and then used for routine follow-up of these patients.
Ultrasound breasts
This is commonly performed as part of the work-up of breast lumps, and can be used to guide needle-biopsy of masses that appear suspicious on the ultrasound.
Ultrasound thyroid
We can use this to assess palpable thyroid nodules, to determine whether they appear benign or warrant a biopsy (called a fine-needle aspirate, or FNA); the FNA can be performed under ultrasound guidance.
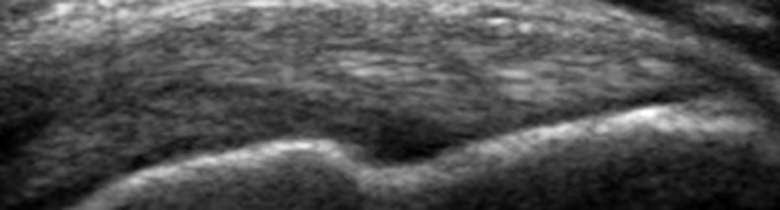
Musculoskeletal Ultrasound
More and more, ultrasound is being used to assess for internal derangement of joints; in many joints, it is as accurate as MRI (the main exceptions being the hip and knee). We can use ultrasound to diagnose synovitis, allowing us to see evidence of diseases such as rheumatoid arthritis at an earlier stage than radiographs. It can be used to assess for tendon degeneration and tendon tears, inflammation of the tendon sheaths (commonly seen in patients with rheumatoid arthritis and psoriatic arthritis), and ligament and muscle tears.
Ultrasound-guided Procedures
Ultrasound is ideally suited to guiding needles into organs, lesions, lymph nodes and fluid because it provides real-time feedback on the position of the needle relative to the target. This allows procedures to be performed rapidly, safely and accurately, without the use of ionizing radiation and with minimal patient discomfort – most of these procedures are performed with local anaesthetic only, or with a combination of local anaesthetic and light sedation with midazolam.
Most lesions in most places can be biopsied using ultrasound, however there are some limitations: as ultrasound cannot see into the lungs or through cortical bone, lung and bone tumours require CT guidance for biopsy. Some deep lymph nodes (for example, retroperitoneal) will also require CT guidance to perform a safe biopsy.
During your rotation with us, you will spend a morning or afternoon in ultrasound. You should use this time to observe one or two diagnostic scans being performed by a sonographer, observe one or two procedures being carried out by the registrar assigned to ultrasound, and to sit in with the registrar while they review and report completed diagnostic scans.